Project Description
A new generation of MR imaging techniques has made it possible to quantify the volume of both whole brain and small brain structures with an enhanced precision, thus allowing a more accurate and detailed assessment of structural brain anomalies in schizophrenia.
Our original study (Shenton et al., 1992, see below), consisting of 15 chronically ill schizophrenics and 15 age-matched normal comparison subjects, reported left-lateralized reductions in gray matter volume in anterior hippocampus/amygdala, parahippocampal gyrus, and superior temporal gyrus of schizophrenics compared with normal controls. This study further showed that the hallmark clinical symptom of thought disorder is associated with a specific reduction in the volume of left posterior superior temporal gyrus gray matter, which encompasses primary auditory cortex and association cortex, including planum temporale, regions long implicated as neuroanatomical substrates of language. After these initial findings, volumetric measurements were made for other regions of interest (ROIs), including prefrontal cortex (Wible et al., 1995, see below), basal ganglia (Hokama et al., 1995), thalamus (Portas et al., 1998) and cerebellum (Levitt et al., 1999). Abnormalities in these other brain regions were also noted although they were not as pronounced as the abnormalities observed in the temporal lobe structures.
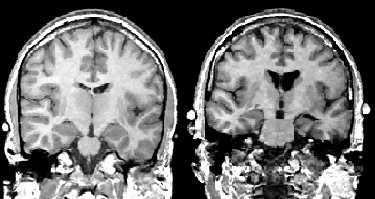
Coronal MR scans from a chronic schizophrenic (right) and normal comparison subject (left). Note increase in CSF in left amygdala-hippocampal complex.
Our group is currently working with a new set of chronically ill patients in order to extend our earlier study. In particular, we are interested in the influence that the clinical symptoms have on MRI morphometry abnormalities. We are also interested in evaluating temporal-frontal pathways in the symptomatology of schizophrenia as well as using new tools such as functional magnetic resonance imaging (fMRI) and diffusion tensor imaging to evaluate brain abnormalities in schizophrenia.






Comments are closed.